At-A-Glance
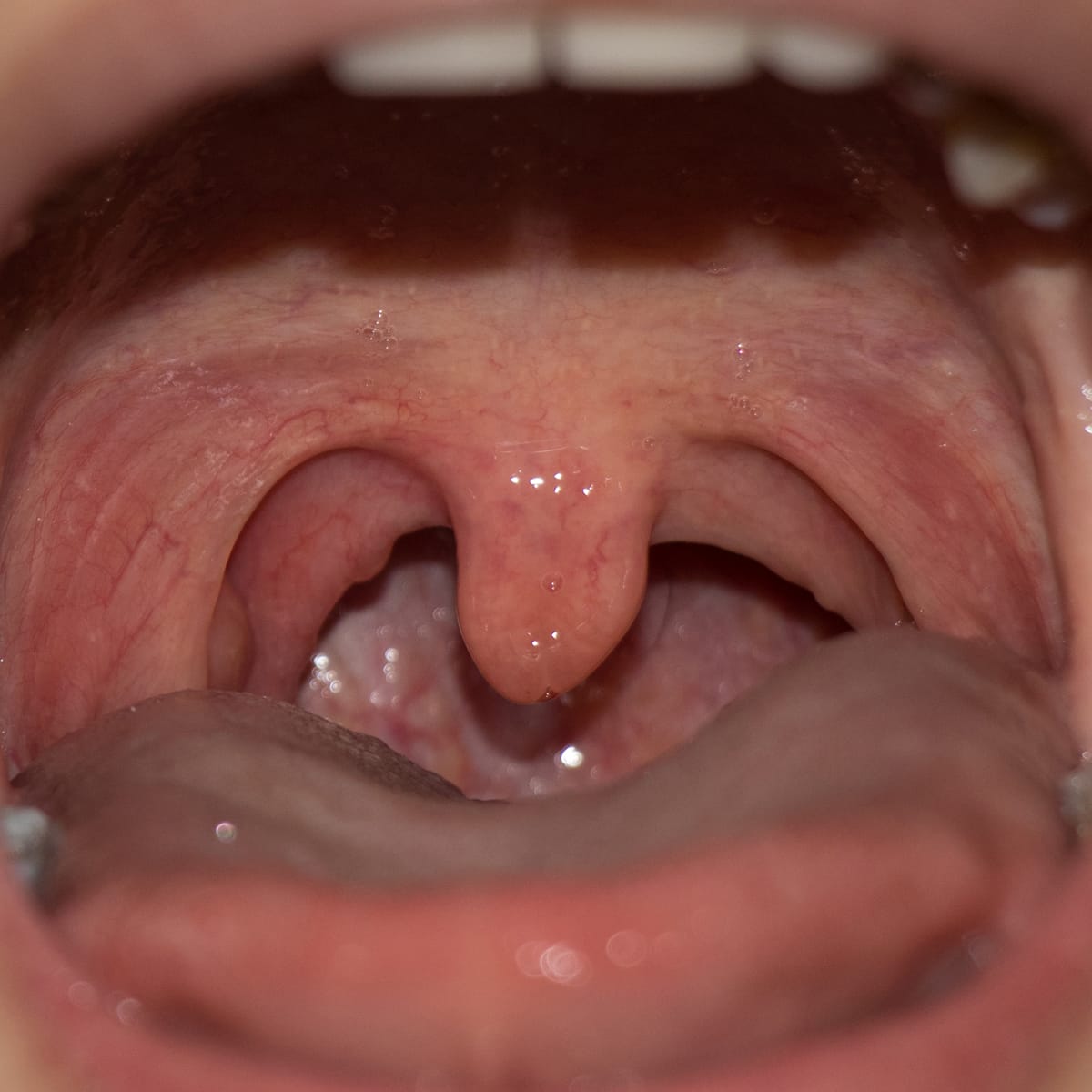
- Even though some people claim that the uvula, the fleshy extension of tissue that hangs down from the middle of the soft palate, can affect speech and swallowing, this is false. Like the appendix, the uvula is a vestigial structure with no function; it doesn’t cause symptoms unless it gets very swollen; and then it can cause a lump-in-the-throat sensation, throat irritation, snoring, choking episodes, and chronic cough.
- Other than trauma, which is rare, the only proven cause of an enlarged uvula is silent nighttime respiratory reflux (aka LPR). Since the underlying problem is reflux, it makes no sense to have surgery to remove the uvula before first undertaking a tight anti-reflux program.
- If the reflux is controlled, the uvula will shrink back to its normal size, usually within weeks. However, if the “bigger” problem is snoring, with or without sleep apnea — also both caused by long-standing silent reflux — resolution with an on-going anti-reflux program may take many months.
- That said, the surgical procedure, UPPP (uvulopalatopharyngoplasty), is usually completely unnecessary for just an enlarged uvula … and it may or may not be indicated for snoring.
What Causes an Enlarged Uvula?

These three photos were taken by the author using an ultra-thin instrument (endoscope) placed through the nose to look down the barrel of the throat (on the inside). The image on the left shows LPR with a slightly enlarged uvula; whereas the middle and far-right images show findings of severe LPR with extremely enlarged uvulas.
The image on the far-right actually shows a massive uvula that is resting on the epiglottis of the larynx (voice box). Not surprisingly, that patient was distressed by a constant, unpleasant feeling of something in his throat with additional symptoms of “throat tickle,” chronic throat-clearing, and cough. On a strict reflux detox program, his uvula shrunk back to normal size in four weeks!
Does a Big Uvula Cause Snoring and Sleep Apnea?
Often an enlarged uvula is associated with a narrow (reflux-caused) throat, which may be associated with snoring and sleep apnea; also see Previous Snoring Sleep Apnea Blog.

These three photos show the upper throat; the left photo of the nasopharynx is normal. The middle photo shows intense reflux in the upper throat in a patient with post-nasal drip and sinus symptoms, as well as sleep apnea. The far right image shows severe, long-standing LPR in a patient with severe snoring and sleep apnea.
These images are shown to emphasize the point that some ENT doctors overlook those findings or think them to be “normal.” It is important to note that the findings of LPR are not taught in most physicians’ curricula.
Which Doctor Can Best Diagnose My LPR?
Still, the answer is the otolaryngologist (ear, nose, and throat doctor) even though ENT doctors seem to fall into two camps: one group thinks everyone has reflux while the other thinks that no one has it. Why is this? I believe that reflux findings are so common that they may be mistaken for “normal.”

These photos were again taken by the author using an ultra-thin instrument (endoscope) placed through the nose to look down the barrel of the throat. The image on the left shows a normal larynx; note the sharpness of the vocal cords, the “V-shaped” structures in the middle. The two other images show LPR in which the vocal cords are very swollen like sausages. Also, in the middle image the back of the larynx (at the top of the photo) is obviously swollen as well. And the image on the far- right shows that the back of the larynx is so swollen that it is actually in contact with the posterior pharyngeal wall, (the back of the throat).
Notably, the far-right image is taken from a patient with long-standing nighttime reflux, and symptoms of globus, chronic throat-clearing, dysphagia (difficulty swallowing), and hoarseness as well as snoring and sleep apnea. This is severe LPR.
In part, I have included images in this post so that you can print them to show your ENT doctor … with the question, “Do I look like this?”
What Can I Do About My Enlarged Uvula?
Adopt a strict antireflux program for four weeks: (1) no eating within five hours of bedtime (lying down); (2) sleep up at a 45-degree angle; (3) low-fat, low-acid diet; (4) famotidine 20 mg. before breakfast and dinner, and 40 mg. before bed; (5) a swallow of Gaviscon Advance Aniseed after dinner and before bed; (6) gum chewing after eating; and (7) alkaline water.
Note: I never recommend PPIs and all of these topics/elements are covered in greater detail throughout this blog site; see Silent Reflux, Is a Vegetarian Diet Good for Reflux, and Respiratory Reflux,
Who Should Have the UPPP Operation?
In my opinion, very few people need surgery … assuming that the patient takes their anti-reflux program seriously. Again, I think UPPP (uvulopalatopharyngoplasty) is not indicated for people with just an enlarged uvula. For those with snoring, with or without sleep apnea, an antireflux trial program is indicated for three months before making the decision to have surgery.